Tooth Discolourations and Bleaching
On 11-12-2019 | Read time about 3 Minutes
Dr. Grossman highlights the major causes for tooth discoloration as:
- Decomposition of the pulp tissue
- Excessive hemorrhage following pulp removal
- Medicaments
- Filling materials
- General systemic conditions
DENTIST-RELATED CAUSES
- Pulp Tissue Remnants
The tissue remaining in the pulp chamber disintegrates gradually and may cause discoloration. Therefore, pulp horns must always be included in the access cavity to ensure removal of pulpal remnants and to prevent retention of sealers at a later stage. Intracoronal bleaching in these cases is usually successful.
- Intracanal Medicaments
Several intracanal medicaments can cause internal staining of dentin. Phenolics or iodoform-based medicaments sealed in the root canal and chamber are in direct contact with dentin, sometimes for long periods, allowing penetration and oxidation. These compounds have a tendency to discolor the dentin gradually. Intracoronal bleaching may be used to correct the problem.
- Obturating materials
This is a frequent and severe cause of single tooth discoloration. Incomplete removal of obturating materials and sealer remnants from the pulp
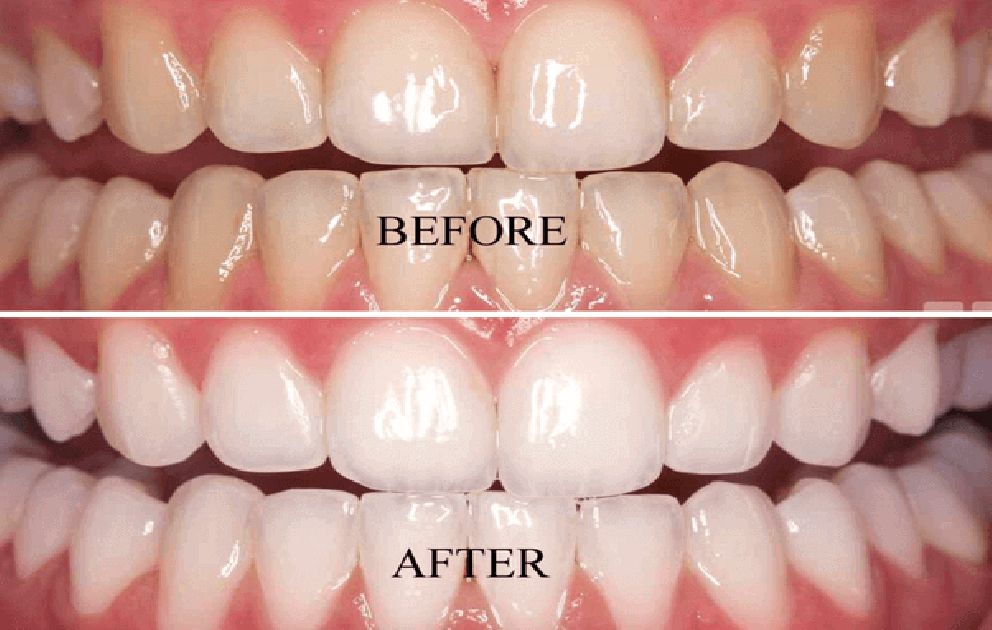
Bleaching of Discoloured tooth
Substances to reverse the stained tooth structure consist of powerful oxidizing agents such as pyrozone (25% solution of hydrogen peroxide in ether), superoxol (30% solution of hydrogen peroxide), and sodium dioxide (yellowish amorphous powder). In an attempt to restore the translucency to the tooth- It is also cited by Dr. Grossman the recommendation of an 80% solution of chloral hydrate that had an index of refraction same as that enamel.
Lightening vital teeth
Generally, most tooth whitening is done with home bleaching kits using custom tray fabrication. In-office techniques are suitable for some patients based on the type and intensity of stain and temperament and wishes of the patient. Home treatment requires compliance and patience, whereas chairside techniques are faster, but often more costly. Direct composite or laboratory porcelain veneers are the next most conservative approach and may be used when bleaching does not produce satisfactory results. Veneers are also useful when the shape, size, or arrangement of teeth is aesthetically unacceptable. Finally, full-coverage porcelain and porcelain fused to metal crowns are the most invasive methods; these may be used when there is a need to replace damaged or missing tooth structure.
- Tetracycline Stains
Administration or ingestion of certain drugs during tooth formation may cause severe discoloration. Correction of tetracycline-stained teeth may pose a clinical challenge. For mild to certain moderate cases, repeated external bleaching for an extended period can be effective. However, severe cases, especially those of dark gray color, should be corrected by restorative means.
BLEACHING MECHANISMS
INTRACORONAL BLEACHING OF ENDODONTICALLY TREATED TEETH
- Walking Bleach
The walking bleach technique should be attempted first in all cases requiring intracoronal bleaching.
- Thermocatalytic
This technique involves placement of the oxidizing chemical, generally 30% to 35% H2O2 (Superoxol), into the pulp chamber followed by heat application either by electric heating devices or specially designed lamps.
COMPLICATIONS AND ADVERSE EFFECTS FROM INTRACORONAL BLEACHING
- External Root Resorption
- Chemical Burns
- Inhibition on Resin Polymerization and Bonding Strength
EXTRACORONAL BLEACHING
Extracoronal bleaching may be used for whitening vital or nonvital teeth as well as a single tooth or whole arch.
- In-office Extracoronal Bleaching
In-office bleaching materials are almost exclusively in the form of a gel, with 25% to 38% H2O2.
- At-home Extracoronal Bleaching
For professional at-home bleaching, custom tray technique is most commonly used. The bleaching gel is loaded in the tray, and the patient wears the tray for several hours up to overnight daily usually for 2 weeks or until a satisfactory tooth shade is achieved. Both H2O2 and carbamide peroxide are used as active ingredients for professional at-home bleaching products, mostly containing 3% to 7.5% H2O2 or 10 to 22% carbamide peroxide, with latter, especially those with 10% carbamide peroxide, being more popular.
COMPLICATIONS AND ADVERSE EFFECTS FROM EXTRACORONAL BLEACHING
- Tooth Sensitivity
- Enamel Damage
- Gingival Irritation
- Mercury Release from Amalgam Restorations

FREE PROMETRIC PRACTICE TESTS
Try out the most relevant Prometric mock test questions for Dental exams here.
ENROLL NOW